Diabetes Leg Pain: Could It Be Peripheral Artery Disease (PAD)?
Share IT

Launch Your Dream Website with Us!
Click Here to Get in touch with Us.
Categories
Diabetes Leg Pain
Diabetes and Peripheral Vascular Disease (PVD): Taking Care of Your Feet and Legs
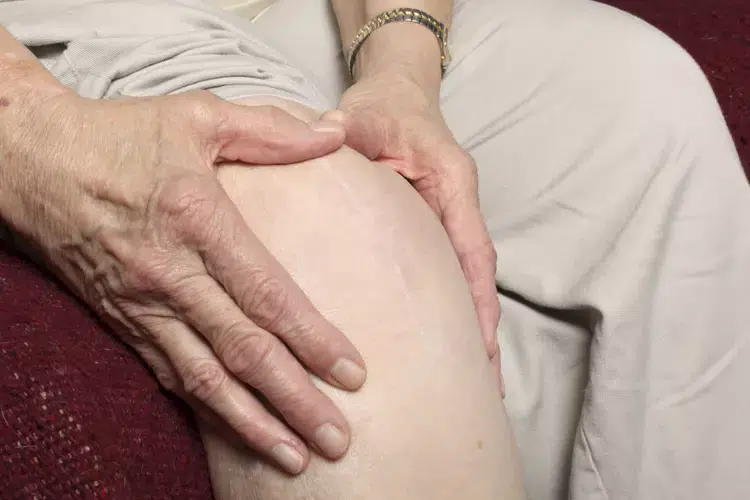
Peripheral vascular disease (PVD), also known as peripheral arterial disease (PAD), is considerably more likely to occur in people with diabetes. PVD is a disorder that develops when plaque accumulation (atherosclerosis) causes the arteries in the legs and feet to constrict or obstruct. In severe situations, this reduced blood supply can result in amputation and tissue death in addition to discomfort, cramping, and numbness. For problems to be avoided and your legs’ good circulation to be maintained, early detection and treatment are essential.
Thank you for reading this post, don't forget to subscribe!Diabetes Leg Pain
Table of Contents
The Man Behind the Scenes: How Diabetes Causes PVD
Diabetes Leg Pain
Diabetes’s elevated blood sugar levels cause PVD in a number of ways, including:
- Accelerated atherosclerosis: The inner lining of arteries is damaged by persistently high blood sugar, which increases the artery’s susceptibility to inflammation and plaque accumulation.
- High levels of blood fat and sugar: Plaque accumulation is accelerated by high blood sugar in addition to raised levels of triglycerides (blood fats) and LDL (“bad”) cholesterol.
- Reduced blood flow: As arteries constrict, there is less blood flow to the legs and feet, which depletes the tissues’ supply of nutrients and oxygen.
A Range of Indications: Understanding PVD Signs
Diabetes Leg Pain
In its early stages, PVD can progress silently without exhibiting any symptoms. But if the illness gets worse, you could encounter:
- Leg Pain: The most prevalent symptom of PVD is leg discomfort, which is frequently reported as cramping, aching, or a burning feeling in the calves and legs. Claudication is a pain that usually flares up with exercise and goes away with rest.
- Numbness or tingling: The legs and feet may also experience numbness or tingling.
- Weakness: Muscle weakness in the afflicted legs may result from decreased blood supply.
- Skin colour changes: Due to inadequate circulation, the skin on the legs and feet may seem pale or bluish.
- Wounds that heal slowly: Due to inadequate blood supply, open sores on the legs and feet may not heal at all or may take longer to cure.
- Leg colds: Due to decreased blood flow, the afflicted leg or foot may feel cooler than the other.
When to Get Assistance: Prevention Preserves Limbs
Diabetes Leg Pain
See your doctor right away if you have any of these symptoms, especially if you have leg pain when moving around. To control PVD, avoid complications, and safeguard your legs and feet, early diagnosis and treatment are essential.
Putting Up a Front: Lifestyle Techniques for Proper Circulation
Diabetes Leg Pain
You may greatly lower your risk of PVD and enhance circulation in your legs by leading a healthy lifestyle:
- Maintain appropriate blood sugar control: Reducing the risk of PVD and improving general diabetes health depend on maintaining blood sugar levels within your goal range.
- A balanced diet high in fruit: vegetables, whole grains, and lean protein is recommended for a healthy diet. Limit your intake of added sugars, cholesterol, and saturated and trans fats.
- Frequent physical activity: Aim for 150 minutes or more per week of moderate-to-intense activity or 75 minutes or more of vigorous exercise. One particularly useful exercise for enhancing leg circulation is walking.
- Keep your weight in check: Being overweight strains your heart and blood vessels more.
- Quitting smoking: Smoking raises the risk of PVD problems and considerably impairs blood flow.
- Good foot hygiene: It’s crucial to check your feet every day for cuts, blisters and sores. To safeguard your feet, practise good hygiene and wear appropriate footwear.
Options for Treatment: Taking Care of PVD at Different Stages
Diabetes Leg Pain
The severity of PVD determines the course of treatment. Here are a few typical methods:
- Lifestyle changes: Adopting the above-mentioned healthy lifestyle habits is the cornerstone of PVD management.
- Medications may be administered: including drugs that decrease cholesterol and those that increase blood flow.
- Angioplasty and stenting: To open constricted arteries, less invasive techniques may be employed in some situations.
- Surgery: to open a new channel for blood flow around clogged arteries may be required in extreme circumstances.
Managing Diabetes Well: Lifelong Foot and Leg Protection
Diabetes Leg Pain
You may lower your risk of PVD issues and preserve healthy circulation in your legs and feet by making appropriate diabetes control, healthy lifestyle choices, routine doctor’s checkups, and correct foot care a priority. Here are a few more pointers:
- Become knowledgeable: Being aware of PVD and its dangers enables you to take preventative measures to safeguard your feet and legs.
- Be open with one another: Talk to your doctor about any worries you have regarding leg discomfort or circulation.
- Retain a cheerful attitude: In PVD, early identification and treatment can greatly enhance results.

Launch Your Dream Website with Us!
Click Here to Get in touch with Us.

























































Recent Comments