HIV/AIDS in High-Income Countries: Unequal Access Despite Wealth
Share IT

Launch Your Dream Website with Us!
Click Here to Get in touch with Us.
Categories
HIV/AIDS disparities in high-income countries
HIV/AIDS in High-Income Nations: A Paradox
High-income nations continue to struggle to guarantee PLWHIA (people living with HIV/AIDS) fair access to care, despite tremendous progress in HIV therapy. This disparity draws attention to the intricate interactions that exist between insurance coverage, societal determinants of health, and healthcare systems.
Thank you for reading this post, don't forget to subscribe!Table of Contents
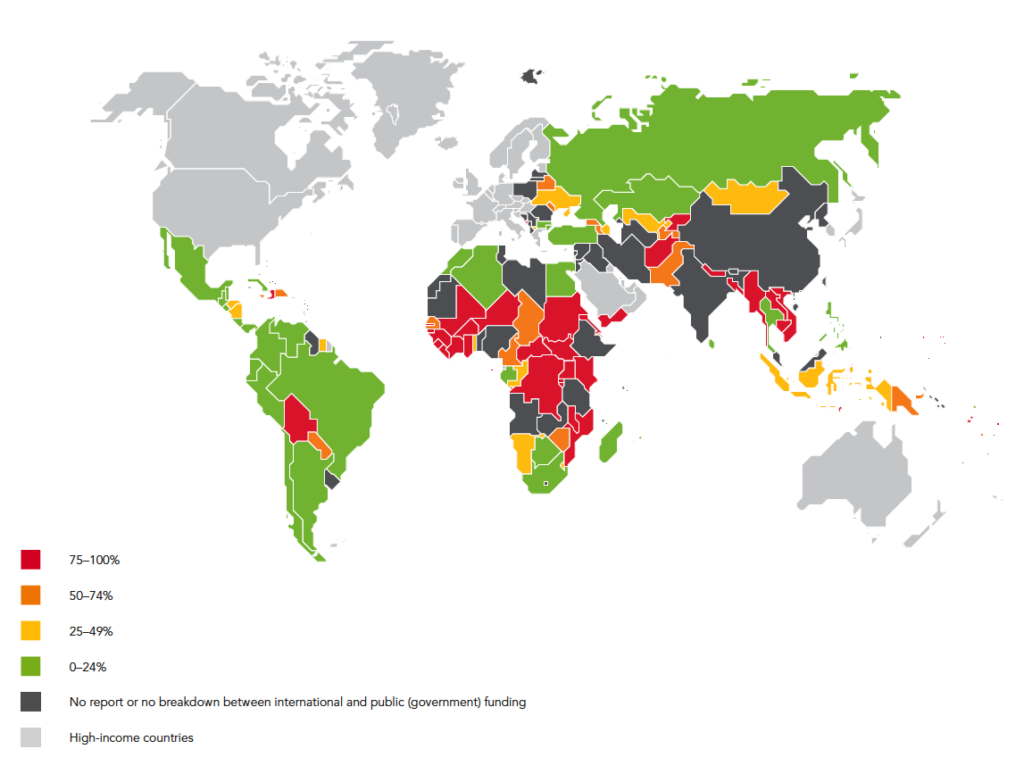
Healthcare Inequalities: A Chronic Issue
HIV/AIDS disparities in high-income countries
People with HIV/AIDS from marginalised populations frequently have worse health outcomes, even in wealthier countries. These differences result from a number of factors:
- Socioeconomic Status: People with low incomes may find it difficult to pay for deductibles, co-pays, or prescription drugs that aren’t covered by insurance. Food insecurity and unstable housing might make treatment compliance even more difficult.
- Race and Ethnicity: In high-income nations, there is generally a greater prevalence of HIV infection and less access to care for racial and ethnic minorities. Historical and current social injustices, such as prejudice in healthcare settings, might be blamed for this discrepancy.
- Gender Identity and Sexual Orientation: People who identify as LGBTQ+, especially transgender women and men who have sex with men (MSM), may encounter prejudice and discrimination in healthcare institutions, which deters them from getting tested and receiving treatment.
- Geographical: Access to specialised HIV care professionals and support services is frequently restricted in rural locations.
HIV/AIDS disparities in high-income countries
These differences result in greater mortality rates among marginalised people, lower rates of viral suppression (undetectable viral load), and delayed diagnoses.
The Function of Insurance Protection
HIV/AIDS disparities in high-income countries
Access to HIV therapy is made possible in large part by health insurance. However, there are two sides to coverage:
- Underinsured and Uninsured: People who are underinsured or do not have enough coverage may find it difficult to afford medical care. Treatment discontinuations and worse health outcomes may result from the high expense of antiretroviral medication (ART) and other necessary services.
- Getting Around in Complex Systems: Getting around in complex healthcare systems can be difficult, even with insurance. For certain individuals, comprehending coverage specifics, prior authorizations, and referrals can be quite challenging.
HIV/AIDS disparities in high-income countries
Additionally, certain insurance plans might only cover a portion of certain HIV-related therapies, such pre-exposure prophylaxis, or PrEP, which prevents HIV infection.
Barriers to Accessing Healthcare Outside of Insurance
HIV/AIDS disparities in high-income countries
Beyond financial constraints, PLWHIA encounter other challenges. Health-related social variables have a big influence on care access:
- Stigma and Discrimination: People may be discouraged from obtaining testing and treatment if they fear stigma and discrimination in healthcare settings. Overcoming this obstacle requires creating environments that are inclusive and welcoming.
- Transportation Difficulties: It may be challenging to gather prescriptions and attend routine clinic visits if there is a lack of dependable transportation. For people living in rural areas, this issue is especially serious.
- Mental Health Needs: Anxiety, depression, and other mental health issues are common in PLWHIA. The general well-being and adherence to treatment might be adversely affected by inadequate access to mental health treatments.
- Language Disparities: Inadequate availability of translators and culturally aware medical professionals might impede effective care by causing communication breakdowns.
The Way Ahead: Achieving Equitable Access
HIV/AIDS disparities in high-income countries
To tackle these differences, a multifaceted strategy is needed:
- Enhancing Public Health Initiatives: It is imperative to increase the number of people who have access to low-cost or free HIV testing, treatment, and prevention services (such as PrEP).
- Targeted Outreach and Education: It is crucial to implement programmes that provide culturally relevant information and education on HIV prevention, testing, and treatment to underserved areas.
- Policy Advocacy: Advocating for policies that reduce cost-sharing for necessary HIV services, increase insurance coverage, and address socioeconomic determinants of health can have a big impact.
- Fighting Stigma: It is critical to support programmes that raise public knowledge about HIV and work to lessen prejudice and stigma in both the healthcare industry and society at large.
- Investing in Community-Based Care: It is crucial to assist community healthcare organisations that offer PLWHIA accessible and culturally appropriate services.
HIV/AIDS disparities in high-income countries
High-income nations can go closer to realising the objective of universal access to HIV prevention, care, and treatment by addressing these issues.

Launch Your Dream Website with Us!
Click Here to Get in touch with Us.

























































Recent Comments